
A bout of flu turned life-threatening for Nicole Barnes, but the generosity of organ donors has given her a life she never knew existed. She spoke to KATRINA LOVELL about her journey during organ donor week.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
When a holiday to sunny Queensland turned life-threatening for Warrnambool's Nicole Barnes it was the start of a two-year journey that resulted in a lung and kidney transplant.
A heel prick test done shortly after birth revealed Nicole had cystic fibrosis - an inherited condition which primarily affected her lungs and digestive system.
While her lung function had started to deteriorate in the years leading up to that trip to Port Douglas in 2017, the doctors hadn't got to the point of discussing a lung transplant, but she knew it was probably something that was "in the not too distant future".
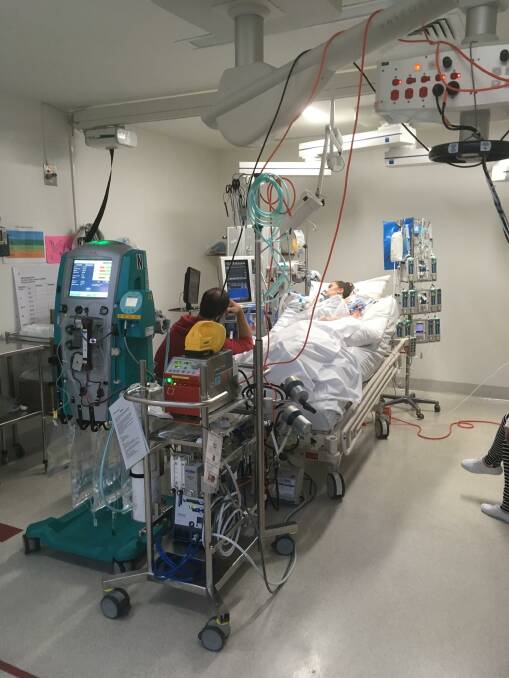
But what happened on that trip ended up taking Nicole close to death, putting her in hospital for 250 days of the next year - 120 of them in ICU - and left her having to learn how to walk again.
One day they were walking on the beaches an hour, the next both Nicole and her husband Ian could barely get out of bed - something that was unusual for Ian who regularly competed in triathlons.
"We knew it wasn't good," Nicole said.
When they called The Alfred hospital in Melbourne, Nicole was told to take some Tamiflu tablets, but the chemists had sold out.
So they flew home early and went straight to The Alfred where Nicole spent the next month battling the flu.
"That was pretty scary from the word go. I'd never had to use oxygen before," she said.
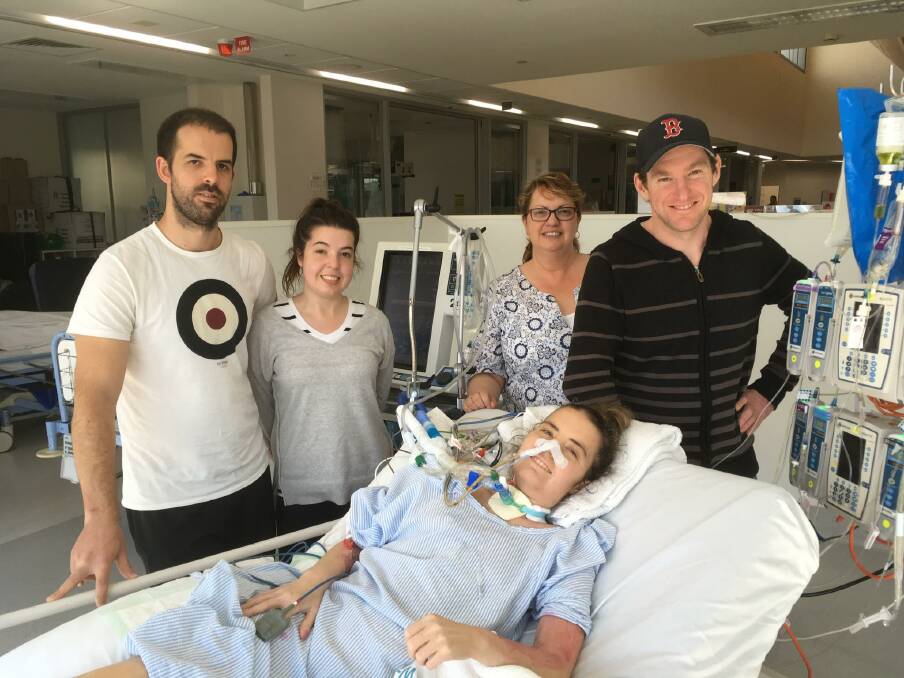
After two weeks of antibiotics, she started to pick up but a couple of days later things started to go downhill again when pneumonia set in. Nicole doesn't remember much after that.
"It went from scary to worse," Ian said. And that's when doctors started to talk about Nicole not making it through.
She was put on life support in ICU while she waited for an emergency lung transplant - a wait that usually takes a few months at best. "We didn't really have that time," Ian said.
As well as being on a ventilator, Nicole was put on an ECMO machine. "It's a pretty scary machine considering I spent the Tuesday morning Googling 'what's an ecmo machine?'," Ian said.
"It basically takes the blood out of your legs, spins it and takes the carbon dioxide out and puts the oxygen back into it. It does the full job of your lungs.
"You're stuck in bed, you can't move your legs."

The call went out nationwide and within five days the call came through they had found a donor.
"It was really exciting for us but always mixed emotions at that point because you know what that means for another family and that's kind of tough," Ian said.
"Knowing that in our excitement or joy another family is going through the deepest of sadness and horrible time.
"We were so thankful that a family had made a decision to donate a loved one's organs during such a difficult time and give Nic a second chance."
A standard operation usually takes six to eight hours, Nicole's took 13. "She required 100 units of blood during the whole thing. It was quite a scary time and definitely not what you'd call a simple one," Ian said.
While most people come off the ECMO machine after the surgery, Nicole had to stay on it for another four weeks to help her lungs repair.
An ICU stay after a lung transplant is usually only a week, Nicole was there for months.
After the surgery, a number of infections threatened her recovery. "It was a nasty time for Ian and my family. A few times they got told 'we can't do anything else'," Nicole said.
"I was told a few times to prepare and that Nic may not see the day out," Ian said.
"We just held hope. We knew Nic was not someone who ever gave up and fought like hell, even if she didn't realise, that's what she was doing."
Being confined to a bed and hooked up to machines for so long left Nicole "not being able to do anything".
Her muscle had all disappeared, and was down to about 38kg, Ian said.
The first physio session after she was well enough involved having four people helping her to sit up in bed for 10 seconds.
"Nic basically had to re-learn to walk again," Ian said.
Nicole had been so sick that when she came off the ECMO machine, her kidneys didn't "wake up"
So as well as three days a week of intense lung transplant rehab gym sessions to learn to walk and get her lungs functioning properly, she also now needed dialysis three times a week for four to five hours.
Dialysis is different for everyone, and with Nicole's kidneys not functioning at all that meant sticking to a diet that could include just 750mls of fluid a day from both food and drink.
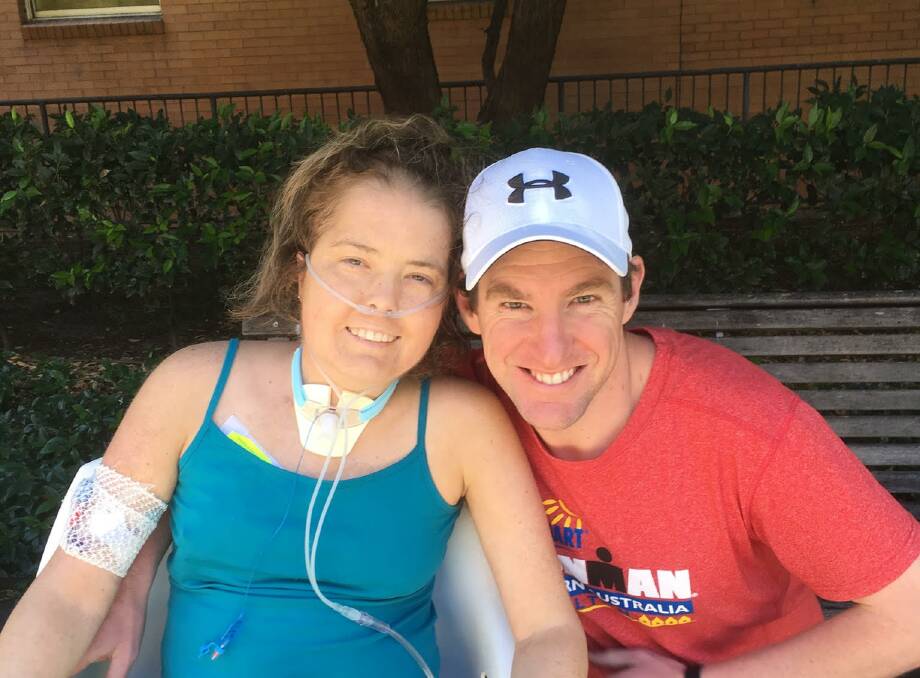
Fluid can sit on your lungs and cause pneumonia, and there is only so much fluid dialysis can remove without you "crashing", Nicole said.
It was a full year before Nicole was able to return home to Warrnambool in July 2018 while she awaited a kidney transplant - with the doctors predicting a five to seven-year wait on a list 1000 people long.
Without telling Nicole, Ian asked the doctors what it would take for him to donate one of his kidneys to Nicole and he started undergoing intensive testing to see if it was possible.
Initially, tests showed he could donate his kidney to her, but the final round of testing showed she would likely reject it straight away.
"It was a devastating blow at the time. A lot of that was, in part, because with the lung transplant I'd had so many blood products which give you a lot of antibodies and they are kind of like the enemy of transplants," Nicole said.
So they signed up to the Paired Kidney Exchange Program - a program to help 'pairs' exactly like Nicole and Ian. A person in need of a kidney who has a willing donor but is not a match is paired with a couple which does match for a "swap" of kidneys. Expecting a long wait on the program, luck went their way, and a match was found the first time their names were entered into the program.
It ended up being a simple two-way swap, she said, but for others it can involve swaps between seven or eight people across multiple states, even New Zealand.
"In the end I have someone else's kidney and someone else has Ian's," Nicole said.
"It's a nice feeling that we've helped another couple as well," Ian said.
After 20 months of dialysis, Nicole's kidney transplant was set for May 2019 but the surgery almost didn't happen.
The night before the surgery, someone had turned off the air-conditioning in the operating theatre, delaying the surgery for a couple of hours. And with both Ian's and the donor's surgery timed for exactly the same time, they were lucky it didn't have to be cancelled because that would have meant at least another three-month wait to coordinate two hospitals, four different surgeons and four surgeries while hoping one of the four patients didn't get sick and make the "chain fall over".
For Nicole, the difference the surgery made was instant. "Within two days it was so hard to describe. It was like a fog had been lifted," she said.
"I never quite realised how sick and debilitated I was. Once I had the lung transplant I thought that was my new normal but it wasn't until I had the kidney that I actually realised how ill I was feeling from not having a kidney.
"My breathing. I guess I've got used to it now but it's just strange breathing and not feeling the labour of breathing. You just do it and there's not a cough."
Before the transplants, Nicole would fall asleep on the couch each night before 8pm exhausted from the day. She now enjoys while getting out for exercise being able to chat the whole way to Ian because she isn't fighting to just breathe at the same time. "I have had a few friends comment, 'gee you don't shut up these days'," Nicole said.
In October, she was able to go back to work. Their plans to finish off that 2017 holiday in Port Douglas this year were scuttled by the pandemic lockdowns.
Since March they have been working from home, catching up with family and friends on Zoom and doing their shopping online.
"We're just staying home and staying safe. I am immune suppressed so that my body doesn't reject the lungs and kidney, and it does make me more vulnerable to things like COVID," Nicole said.
"It's hard to see people do the wrong thing. There's others to think of not just yourself."
Telehealth has meant they haven't had to do all the trips to Melbourne for check-ups.
"For close to 10 years I haven't had so much time away from hospital," Nicole said. She also hasn't had an admission to hospital for treatment since November last year - a record-breaking stretch.
"I'm doing activities I could never do before," she said.
Nicole has also been able to take up Pilates - something that before the transplants would have made her start coughing up blood.
Growing up a persistent cough was the telltale sign of her CF, but she credits her mum with giving her a positive mindset about her illness. "I was brought up to make it part of our lives, not our lives," she said.
Her routine in the years leading up to the surgery would involve two to three hours of physio and exercise two to three times a day in between work.
She'd also have up to 20 tablets a day to help her digest her food because her pancreas doesn't work properly.
Six of the 12 months of every year was spent on IV antibiotics for chest infections that would pop up - the older she got the course of antibiotics was needed for longer and more often.
"No one other than Ian really understood the time and effort involved just to stay well," she said. "I was pretty good at hiding it from those around me"
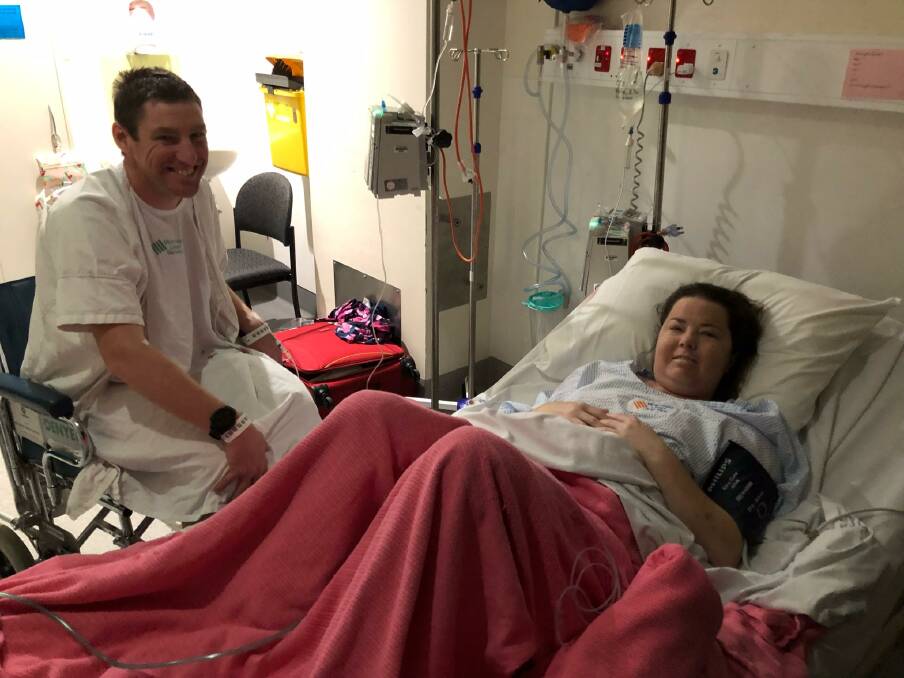
"Each morning I would get up and clear a coffee cup full of thick sticky mucous out and then get on with the day and do the same at the other end of the day. An important part of my routine was exercise to keep what was left of my lungs functioning, although the ability to do this was limited by my limited lung capacity.
"My new lungs don't technically have CF anymore. I don't have a cough anymore. There's nothing to clear out. I've just got normal person lungs now.
"Going from three hours of physio and nebulisers a day to nothing is strange to have all that time back. And now with so much energy, it is often Ian saying 'probably should go to bed' come 11pm at night."
Nicole has written to her anonymous donor, and the couple encourage everyone to have a chat with their families about their wishes around organ donation, as ultimately in the event of something going wrong it is your family that make that decision for you.
"It's terrible to turn one tragedy into two tragedies. If you can make that decision of donating an organ it can change someone's life," Ian said.
Nicole said that while the anonymous lung donor saved her life, it was Ian's gift that gave Nicole her life back.
To find out how you can register your wishes to be an organ donor please go to the Donate Life Website.

