Beds are sitting vacant at Warrnambool's private hospital while the region's major public hospital is bursting at the seams.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Warrnambool Base Hospital has outgrown its intended capacity by more than 10,000 patients per year as numbers continue to climb.
As the major provider and specialist referral centre for the 110,000 people in the south-west Victoria catchment, the hospital continues to face severe capacity constraints, particularly in the emergency department, theatre suites and mental health.
Meanwhile, private services are feeling the sting of declining health insurance uptakes and are struggling to fill beds.
Hospital awaits upgrade

There is a strong push for government funding for stage two of the base hospital upgrades, which would include the construction of a four-level clinical tower with a new emergency department and operating theatres. The current three operating theatres would increase to six, while emergency department cubicles would expand from 19 to 38.
The building would also contain a 32-bed inpatient unit, a paediatric unit, a 12-chair dialysis unit and centralised sterilising and pathology departments.
Each annual report for South West Healthcare from 2003 carries a similar narrative: "The organisation continues to face the challenge of dealing with record levels of patient demand".
In the past 10 years, inpatient numbers have risen dramatically at WBH from 13,858 to 21,425.
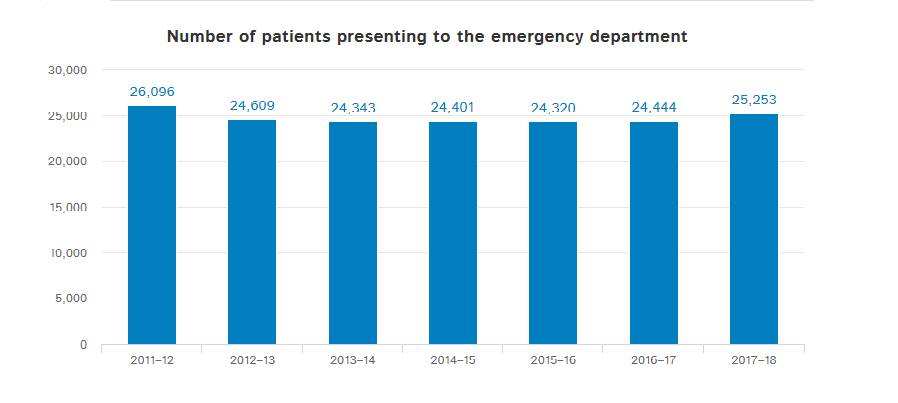
More than 25,250 patients presented to Warrnambool's emergency department in the year ending June 30, 2018.
Latest figures show that of the more than $5.2 million made in patient fees by South West Healthcare, another $1.8 million was made just through admitting and charging private patients.
Some reports in that time show more patients were treated by "using less bed days", with average hospital days cut from 3.4 days to 2.6 days in five years.
"In the last three years, South West Healthcare has seen 30 per cent more patients treated through our acute facility which has, in part, contributed to our budget, staffing and services almost doubling in the past decade," South West Healthcare CEO Craig Fraser wrote in the latest annual report.
"Activity highlights more than 150,000 treatments were provided across our regional and campus-based services; 23,683 inpatients were cared for (a 5.7 per cent increase on 2016-17) and 7658 patients had surgery.
"Our mental health services worked across the region to deliver 2642 episodes of care to new and existing clients (equal to more than 32,000 hours of direct care) whilst patient numbers at our primary and community services, including our dental, general practice clinic, campuses and allied health services, soared to a combined 92,452."
Mr Fraser said the multi-million dollar stage two upgrade of the hospital was needed to deliver safe and effective care.
"It (the upgrade) includes new theatres, emergency department, inpatients wards and underground car park, enabling us to meet increasing demand," he said.
"Planning for the delivery of this project continues as we aim for state and federal government funding commitments to proceed."
Cashing in on private patients

Public hospitals, pressed for productivity while on tight operating budgets set by state governments, actively seek other sources of funding, including insurance payments.
St John of God Hospital Warrnambool chief executive officer Jo Bell said private patients were seeking treatment at public hospitals to avoid paying excess fees.
She said if a private patient chose to be treated in a public hospital, the public hospital would receive funding from that insurer which they would not otherwise receive.
"Every public hospital in Australia is doing that, absolutely, because they get the revenue from taking private patients," she said.
"But they need to be supporting both hospitals. Of course not all patients can be appropriate for us, someone in intensive care needs to stay at the base, and that's how we do work well together.
"But the patients that are appropriate to come here should come here."
They get the revenue from taking private patients
- Jo Bell
She said WBH was running at capacity while St John of God had empty beds.
"Our bed occupancy is just under 50 per cent and that's an issue for us, we need to be higher," she said.
"It's always chockers at the base, we could relieve that pressure.
"We need to remain viable because private hospitals are a very important part of the community.
"There are substantial waiting lists at public hospitals, we have people come here who are happy to pay for procedures upfront with no insurance. The result is that someone doesn't wait three months to have an endoscopy for example.
"It's important the alternative is there."
Ms Bell said St John's biggest struggle in recent times was the drop in private health insurance take-ups.
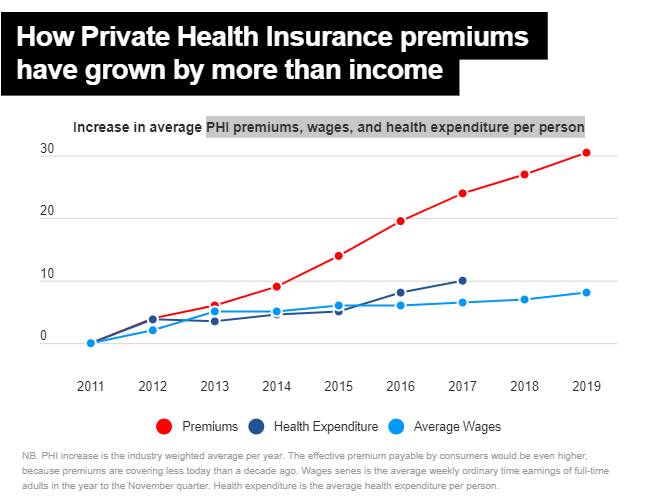
"We're seeing a tangible difference in the number of patients taking up health insurance," she said.
"It's obvious more people are dropping their health insurance or not taking up insurance.
"Because private insurers are doing it tough, the hospitals are also doing it really tough. Private health insurance companies are struggling to give the right amount back to hospitals, and hospitals are suffering.
"It's hard to upkeep a hospital when you haven't got a lot of government support. We're a not-for-profit so we have to use our dollars sparingly, it's really hard at the moment."
The private hospital has just over 200 staff and 74 beds in total.

She said private and public hospitals needed to work together to ensure sustainability into the future.
"We need each other, we both need to be here," Ms Bell said.
"Having a private hospital in the area attracts more doctors to the region because it means they get to work in both areas.
"A good way to recruit medical staff is to offer work in both public and private, and we need to recruit more physicians and general doctors to the area."
Public under pressure

Tim Baker is an emergency specialist at South West Healthcare and is the director of the Centre for Rural Emergency Medicine.
He said public hospitals were often strapped for beds.
"Even though public hospitals like to admit private patients, because they do get paid for them, public hospitals are often very full," he said.
"Most rural hospitals have pressure for beds, and are at capacity, and would like to keep private hospitals full.
"But we have to get someone to look after them in the private hospital too.
"Because private hospitals are often very small, patients often have to be quite well to go there."
He said rural hospitals found it harder to recruit and retain medical staff.
"I think in this region it is really hard to recruit medical staff, both general practitioners and specialists," he said.
"Recruiting doctors can be really hard. I think in Australia in general there's a real geographic narcissism that whatever happens in urban areas is better and anything that happens in rural areas is less good, less quality and less interesting.
"And I think that's really not true, there's some quality services and fantastic medical specialists here. But it's hard to publicise that when the general story seems to be that rural areas lack everything."
I think in Australia in general there's a real geographic narcissism, that whatever happens in urban areas is better, and anything that happens in rural areas is less good, less quality and less interesting.
- Tim Baker
He said the partnership in south-west Victoria between Deakin University and the medical centres was one of the region's best assets.
"It allows for a lot more local specialists, speciality trainees and I feel you get a very similar level of training at South West Healthcare as any other hospital."
He said it was the smaller country hospitals that were often hit the hardest.
"When it comes to difficulty in emergency services, you only have to look at what's happening at emergency services at smaller hospitals like Timboon and Terang, in that they are finding it hard to recruit enough general practitioners," Mr Baker said.
"For a while we didn't train GPs with the full set of skills needed to work in country hospitals.
"A country GP needs to have extended skills compared to an urban GP who works in an office. They need to work in the emergency department, they need to be able to manage people in the hospital as inpatients, they need to deliver babies, some need to give anaesthetics.
"For a long time we didn't have a system of doing that, and now there's a real push to train rural generalists.

"They also have some trouble recruiting highly qualified paramedics to the area, especially Mobile Intensive Care Ambulance (MICA) paramedics.
"Most towns don't have MICA paramedics."
He said one of the most important changes in rural emergency care had been extended care nurses, filling some emergency roles that were previously held by doctors.
He said Warrnambool's medical services were very well connected.
"A real hallmark of Warrnambool's service is connectivity. Safe services are well-connected services," he said.
"I think what we do need is increased cooperation between regional-sized hospitals like Warrnambool and the large urban hospitals when it comes to treating emergency patients.
"Bigger hospitals need to provide more support to smaller hospitals. I think in Warrnambool we do that better than most regions, but I think we can still do better."
'Listen and act', says MP

Member for South West Coast Roma Britnell raised the stage two redevelopment of the WBH in Parliament last month, urging the Premier to listen to the pleas of her constituents.
She handed the Premier a letter from a Koroit patient who suffers a chronic illness and spends six days at the hospital every eight weeks for treatment.
"My constituent knows more than most just how important the stage two upgrade of the hospital is, not only for the healthcare needs of our community but also for the hard working doctors and nurses," Ms Britnell said.
"He sees the pressure the Andrews Labor Government's failure to act over the past five years is having on the facilities, staff and patients."
Ms Britnell said the letter was not a set-up and was a genuine plea for action on the upgrade from a member of the south-west community.
"I have only met this constituent a handful of times - the first when he came to my office and asked me to hand a letter to the Premier," she said.
"If the Premier or his Minister will not listen to me, perhaps they will listen to my constituent, who sees first-hand how desperately this is needed and is now pleading for this important project to be completed.
"Our community has been speaking loudly for the past five years - we want the redevelopment of the WBH completed."
Targeted intervention needed

Lawyer Tom Ballantyne said there were obvious and well-understood reasons why rural Australians often receive poorer health care than those in cities.
The leading medical negligence lawyer and principal with Maurice Blackburn lawyers said rural patients experience a shortage of health professionals, longer waiting times, a lack of health infrastructure, and the tyranny of distance.
"These problems can be solved with the right mix of policies and funding," he said.
"Workforce infrastructure is a critical issue. Building a facility is pointless if you can't staff it appropriately.
"We see this in many regional areas where there is a hospital and an ED but it's being staffed by the local GPs, rather than Emergency Department specialists.
"Regional hospitals can struggle to attract specialists, but this isn't only because of remuneration. It's also related to training and opportunity - many doctors want to be at teaching hospitals for career development."
He said more needs to be done to attract senior medical leaders and administrators to regional areas.
We need targeted and coherent government intervention at all levels. We can't just leave it for the regional health services to work out, it puts too much pressure on them.
- Tom Ballantyne
"We need targeted and coherent government intervention at all levels. We can't just leave it for the regional health services to work out, it puts too much pressure on them," he said.
"In our system, this requires input from federal, state and local governments.
"And importantly, questions have to be asked of the medical and surgical colleges. They also have a role to play.
"We have to ensure the quality of healthcare in rural areas matches that in metropolitan areas - in other words a two-tier system is unacceptable. The legal system doesn't apply a lower standard to medical professionals in rural areas, so why should the patients?"
Have you signed up to The Standard's daily newsletter and breaking news emails? You can register below and make sure you are up to date with everything that's happening in the south-west.


