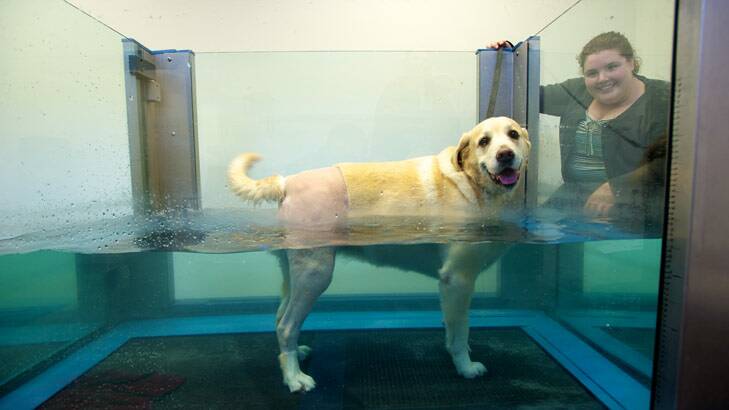
LORELLE Hunt says she would rather ''go homeless'' than see her beloved labrador retriever Rogue suffer. In fact, just last month the Carrum Downs nurse used half the money she had saved for a house deposit to pay for $5000 worth of medical treatment for her nine-year-old dog.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The treatment included stem-cell injections for Rogue's arthritic hips and a knee operation by a specialist orthopaedic surgeon to repair a torn cruciate ligament. And she will pay hundreds of dollars more in the coming weeks for Rogue's rehabilitation treatment, which includes physiotherapy and hydrotherapy.
''I was initially told she was going to need two hip replacements which was going to cost $12,000. I would have paid for it. No question, even though it was my entire savings,'' she says.
''I probably can't afford to buy a house now. But she's like my daughter and I would much rather put that money towards helping my little girl.''
Charles Kuntz, a specialist small animal surgeon who runs Southpaws, the specialist veterinary surgery and cancer facility in Moorabbin where Rogue was treated, says increasingly pet owners are prepared to pay thousands, sometimes tens of thousands of dollars to give their pets the best medical care available.
Recent advances in veterinary medicine mean domestic pets now have access to many of the medical treatments that have long been available to humans, as well as more recent breakthroughs such as stem-cell therapy.
Specialist veterinary cardiologists, for example, can insert pacemakers and less invasive balloon valvuloplasties for dogs and cats with heart disease; oncologists prescribe radiation and chemotherapy for all types of cancers, and some clinics even have their own dedicated oncology ward.
Veterinary neurologists are removing brain tumours, performing radical brain surgery to treat epilepsy and conducting spinal surgery to correct paralysis. Meanwhile, opthamologists regularly remove cataracts from older dogs, and insert artificial lenses to restore eyesight.
But it comes at a price. To treat a dog with cancer, for example, can cost more than $10,000 and up to $20,000 once you factor in CT scans to diagnose the cancer ($1000), surgery to remove a tumour ($3000 to $4500) and follow-up radiation therapy (up to $4500), or chemotherapy ($2000).
Hip replacements cost $6000 per hip; spinal surgery is $5000 and it costs $4500 and $5000 respectively for a knee reconstruction and to have a pacemaker implanted. Dr Kuntz says he once had a client who paid $25,000 to treat a cat for a fungal infection. The treatment prolonged its life by ''two or three years''.
He says while between 20 to 30 per cent of his clients have pet insurance, most pay out of their own pockets.
Alternative and natural therapies for pets are also experiencing a boom. Dr Ann Nevill from the East West Veterinary Group in East Bentleigh treats at least 60 pets a week - from cats and dogs to snakes and turtles - using acupuncture and Chinese medicine.
And Melissa Sciberras from Pawsitive Animal Therapies, provides mobile massage, myotherapy, and reiki healing for conditions ranging from spinal injuries to anxiety for about 40 to 50 patients a week at up to $150 per treatment.
A report by business information analyst, IBISWorld, reveals Australians spent $2.5 billion on veterinary services for their pets in 2011-12 - up from $1.7 billion in 2002-03. That amount is expected to grow by a further 3.7 per cent per year over the next five years to $2.94 billion by 2017, despite an expected decline in the number of pets we own.
Dr David Neck, President of the Australian Small Animal Veterinary Association, says there are several reasons why Australians are spending more on medical care for their pets. At the same time as medical equipment and technology is becoming more readily available, there is a growing demand for specialist veterinary care. ''One of the big shifts has been the availability of technologies that weren't previously available to vets,'' says Dr Neck. ''If you take CT scanners, for example, in the past a vet would have to have a friendly relationship with their local imaging company and at midnight, after all the human patients had gone home, you might be lucky to sneak your dog in.
''Now, around most of the major capital cities there are CT scanners dedicated specifically for pet use and a few of the major centres now even have MRI scanners.''
Dr Neck says this means vets now have a greater ability to diagnose specific conditions and treat them - at a price. ''There's no question that many of our cat and dog owners are demanding more and more for their pets which means vets are under increasing pressure to be right up there with our human medical colleagues in terms of what we can offer.
''But the advances are also being driven by vets themselves because we get frustrated not knowing the answers, or having answers and not being able to fix it. So we actively go out and seek solutions and sometimes those solutions come with a significant cost.''
There has also been a significant rise in the number of vets undergoing specialist training.
According to the Veterinary Practitioners Registration Board of Victoria, the number of registered veterinary specialists in the state - including anaesthetists, radiologists, neurologists, cardiologists and oncologists - has almost doubled in the past decade, from 47 in 2001 to 83 in 2011. There are now five specialist veterinary clinics in Melbourne.
''We're definitely seeing more graduates going on to become specialists,'' says Caroline Mansfield, from the faculty of veterinary science at the University of Melbourne. ''I think they get inspired by the types of cases they see the specialists doing. There is also a lot of really interesting work going on in veterinary medical research right now.''
So much so, she says increasingly the human medical world is looking to veterinary medicine to help better understand and treat some diseases.
''Traditionally, we have often ridden on the coat tails of human medicine. But it seems to be a bit more of a two-way street,'' she says. ''Increasingly we're seeing human medical institutions becoming more interested in seeing what works for us and if it has applications for them.''
Globally, there is a growing movement for ''one health'' medicine where institutions that have both veterinary and human medical departments are more closely aligned.
Dr Kuntz says he was recently contacted by a research fellow from Melbourne's St Vincent's hospital who was interested in the chemotherapy protocols he was using to treat dogs with bone cancer.
There are also social factors that influence how much money people are prepared to spend on their pets.
Pauline Bennett, a neuropsychologist from La Trobe University, founded the Anthrozoology Research Group which studies the relationship between humans and animals. She says: ''There is no question that many more of us value our relationship with our pets more than ever before. Previously, we were so busy with other people that we didn't need pets to fill in all the gaps in our lives,'' she says.
''That's changed. Many of us don't have kids any more … and many of our friends only exist in the digital world. And, of course, if you consider your pet to be a family member then psychologically you have to afford it the same level of care that you would any other member of the family.''
Dr Kuntz agrees. ''I like to say that the dog has moved from back garden, into the living room, into the bedroom and onto the bed. And that's happened over the last 20 years.''
At the same time, he says, there has been a direct correlation with how much pet owners are prepared to spend on their animal's health and wellbeing. Despite this, PetSure's Stephen Owens says ''economic euthanasia'' is the most common cause of death for Australia's cats and dogs, although many vets say pet owners are less likely to ''put down'' the family pet for financial reasons than they were in previous decades.
''We still do see it,'' says suburban vet, Nicole Elias, from Animal Doctors @ Pakenham. ''And it's heartbreaking when it's a decision based on money. But we don't see it anywhere near as much as we used to because our pets are part of the family now much more than they used to be.''
She says an increase in the uptake of pet insurance has also helped.
There are some, however, who wonder whether we should be spending so much money on our pets.
''I think there are some occasions where people do radical treatments and it's not in the best interests of the animal or they feel this economic social pressure to do all they can, even though it means racking up a huge debt or the family having to go without,'' says La Trobe's Pauline Bennett.
Dr Kuntz says it can be a fraught decision. ''You get people sometimes and it's pretty clear that if they elect to have surgery they're not going to be able to buy Christmas presents for their kids and that's a big responsibility on our part. That doesn't mean I'm not going to do it but I'm going to make sure I'm very clear there are other options that may have similar outcomes.'' says Dr Kuntz, who has worked in the US.
''In America, we would get some clients who were absolutely fanatical about going to the nth degree to help their pets, at any cost. But Australians are much more pragmatic.''
Coosje Dubach believes she is one such owner. On the day The Age visits Southpaws, she is dropping off her 12-year-old Weimaraner, Jack, who will undergo surgery that afternoon to remove a cancerous tumour on his lung. Just a month earlier, Jack also had surgery for thyroid cancer. All up, the treatment has cost her more than $9000.
''It was something I had to think about carefully because he is an older dog and I realise everyone has a certain life expectancy. But he is a big part of my life and so, if the surgery can prolong his life for another couple of years then I'm prepared to pay for that,'' she said. ''But I think after this I will let nature do its thing.''
Even Lorelle Hunt, who has taken a month off work to care for Rogue and is sleeping with her on a mattress on the floor because Rogue can't get up on Lorelle's bed, agrees.
''I'd like to think there isn't anything I wouldn't do to help her, no matter how much it cost. But once she gets to her predicted age, then I'd like to think I wouldn't put her through treatment unnecessarily. It will break my heart. But there will come a time when that will have to be it.''
Rachel Wells is consumer affairs reporter.

